Healthcare exists to protect human health, yet the same industry is one of the most emissions-intensive sectors in the global economy. The global healthcare sector generates roughly 5% of the world's greenhouse gas emissions—that's more than aviation. If healthcare were a country, it would be the fifth-largest emitter on the planet. As populations age and demand grows, that footprint will likely continue to increase without action to address it.
For organisations that supply goods or services to health systems, this impacts business. Procurement requirements tied to carbon performance are already in place in the most advanced health systems, and others have plans to follow. This post covers where healthcare's emissions actually sit, how health systems globally are responding, and what suppliers need to have in place as those requirements extend across more markets.
Where do healthcare emissions actually come from?
The answer might surprise most people who haven't looked closely at the data. Hospitals are among the most energy-intensive buildings in the economy, running continuously at controlled temperatures with high-dependency equipment that cannot be switched off, and energy consumption is a significant part of the picture. However, it is not where the majority of healthcare's footprint sits.
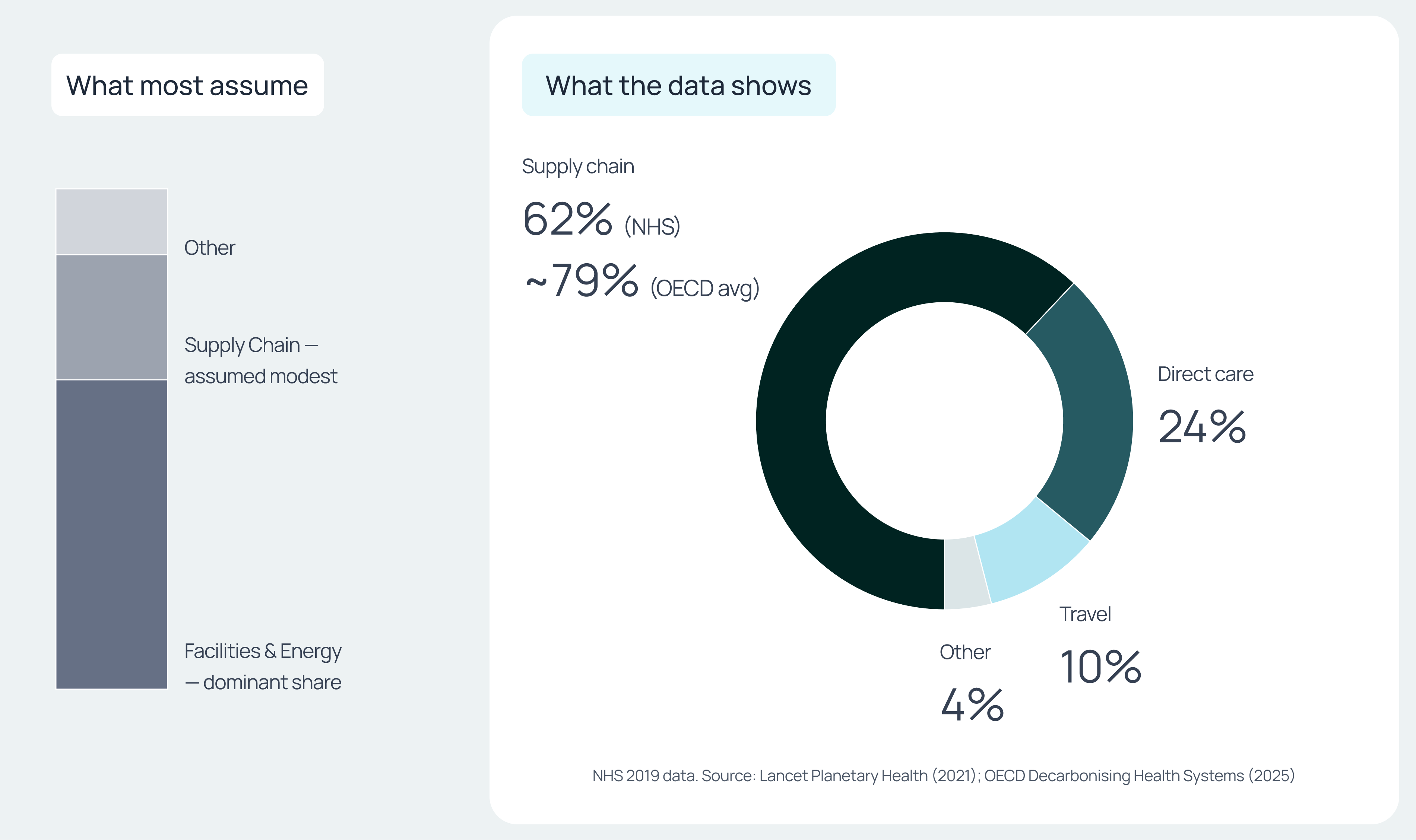
Healthcare itself is a service sector and does not manufacture goods directly, which leads many organisations to assume their footprint is modest, but the supply chain data tells a different story. According to a 2025 analysis, hospitals account for around 30% of health sector emissions on average across OECD countries, but the supply chain is where the real majority sits. Nearly four-fifths of all emissions associated with the health sector can be traced back to supply chains: pharmaceuticals, medical devices, chemicals, logistics, and facilities management.
The NHS is the most comprehensively studied health system in the world on this question. A 2021 study found that the NHS's total carbon footprint in 2019 was 25 megatonnes of CO2e, of which 62% came from the supply chain. Pharmaceuticals and chemicals alone accounted for 32% of the total. Direct clinical delivery—the wards, theatres, and operations most people associate with NHS emissions—accounted for just 24%.
That split matters enormously for anyone supplying healthcare. The majority of the sector's decarbonisation challenge does not sit inside hospitals. It sits in the organisations that make and deliver what hospitals use.
Health systems are moving to act, and procurement is the primary lever
Over 40 countries have now set net zero targets for their health systems, and more than 90 countries have committed to develop low-carbon, climate-resilient health systems. At COP26, 52 countries signed commitments to develop climate-resilient, low-carbon health systems, an initiative that has since grown into the Alliance for Transformative Action on Climate and Health (ATACH), which now brings together over 100 countries working to translate those commitments into delivery. The most advanced programmes offer a clear signal of what others are working toward.
Commitment is building, but the gap between ambition and infrastructure remains wide across most markets. Many health systems have set targets without yet putting the procurement mechanisms, data requirements, or supplier engagement programmes in place to enforce them. That gap will close, and when it does it will close through supply chain pressure.
The NHS: The world's most advanced healthcare decarbonisation programme
In 2020, the NHS became the first national health system in the world to commit to net zero. The targets are structured around the emissions split: net zero by 2040 for the emissions the NHS controls directly, and net zero by 2045 for the emissions it influences through its supply chain. With more than 60% of its footprint sitting in Scope 3, decarbonising procurement is a key priority. The NHS Net Zero Supplier Roadmap is the mechanism for driving this through the supply chain, and it is already in effect. The milestones are binding:
- From April 2022, all NHS procurements include a minimum 10% net zero and social value weighting.
- From April 2024, Carbon Reduction Plan requirements have been extended to cover all new procurements.
- From April 2027, all suppliers will be required to publicly report targets, emissions, and a Carbon Reduction Plan covering global Scope 1, 2 and 3 emissions.
- From April 2028, new requirements will be introduced covering carbon footprinting for individual products supplied to the NHS.
- From 2030, suppliers that cannot demonstrate progress through published reports and continued carbon emissions reporting will no longer qualify for NHS contracts.
Commitment is building, but delivery lags
Health systems account for over 4% of total greenhouse gas emissions in OECD countries, and as populations age and demand for healthcare rises, the sector's environmental footprint is likely to grow without policies to address the issue. Following in the footsteps of the NHS, over 40 countries have set their own net zero targets for their healthcare systems, and more than 90 countries have committed to deliver low-carbon, sustainable health systems. At COP26, 52 countries signed commitments to develop climate-resilient, low-carbon health systems. That initiative has since grown into the Alliance for Transformative Action on Climate and Health (ATACH), which now brings together over 100 countries and areas working to turn those commitments into action.
Although, the gap between ambition and infrastructure remains wide. Many health systems have committed to targets without yet putting the procurement mechanisms, data requirements, or supplier engagement programmes in place to deliver them. Closing that gap will be done through supply chain pressure, not just internal operational change.
How other health systems are structuring their programmes
In January 2024, Danish Regions published a national strategy for sustainable hospitals, with all Danish regions committing to a common goal: reduce hospitals' consumption-based CO2 emissions by 50% by 2035, and achieve net zero before 2050. The strategy explicitly identifies procurement as a primary lever, committing to use targeted procurement activities to stimulate and encourage suppliers and markets to deliver green and sustainable products. This made Denmark one of the first countries to embed supplier pressure directly into a national hospital sustainability strategy.
In the Netherlands, the National Green OR Network, backed by 16 scientific and professional associations, has developed the Green OR Barometer, a measurement tool designed to give hospitals insight into the environmental impact of their operating rooms, intended for rollout across all hospitals in the country. This sits alongside the Netherlands' Green Deal on Sustainable Healthcare 3.0, which has expanded to include the pharmaceutical industry, with over 200 hospitals and care institutions signed up, plus a target of 55% emissions reduction by 2030 and net zero by 2050.
Norway has adopted both an overarching emissions mitigation target for the health sector and eight more detailed sub-objectives aimed at reducing the broader environmental footprint of the health sector while improving health outcomes.
In Austria, a national greenhouse gas calculator is being developed by the Competence Centre Climate and Health, enabling healthcare facilities to estimate emissions using a standardised approach that will allow consistent national reporting. Over 300 institutions have signed up for voluntary support on facility-level decarbonisation.
In Ireland, the Health Service Executive completed a full GHG emissions baseline and decarbonisation roadmap in 2025, developed in collaboration with Health Care Without Harm Europe, outlining the governance, data, and supplier engagement steps needed to transition to net zero by 2050.
What this means for healthcare suppliers
Though healthcare decarbonisation programmes may vary in scope and timeline, the direction is consistent across every market. Health systems that have not yet mandated these requirements are tracking closely behind those that have. The procurement pressure being applied by the most advanced systems today is the model others are building toward, and the timelines are tighter than most suppliers expect. Suppliers that cannot demonstrate credible measurement and a reduction plan are already being excluded from NHS contracts. As equivalent programmes roll out in other markets, the same will apply there.
For most suppliers, Scope 3 emissions make up the majority of their own footprint, and building a credible, auditable inventory takes time. Engaging suppliers for data, establishing defensible methodology, and building a net zero strategy is not something that can be completed in weeks. The organisations best positioned to meet these requirements are the ones that are already building the infrastructure, not the ones waiting for a specific customer to ask for it.
Where suppliers should start
1. Establish your emissions baseline. You cannot build a credible carbon reduction plan without knowing where your emissions sit. Start with Scope 1 and 2, then prioritise the Scope 3 categories most material to your operations, for most healthcare suppliers, that means purchased goods and services and upstream transportation.
2. Map the reporting requirements of your key customers. Leading health systems already require carbon reduction plans as a condition of procurement, with global emissions reporting and product-level footprinting following on fixed timelines. Know your customers' timelines before they become urgent, and treat the most advanced programmes as a proxy for where others are heading.
3. Build your supplier engagement process. Full Scope 3 reporting means data from your suppliers, not just your own operations. That takes time to collect accurately. Start outreach early, use structured templates, and treat supplier engagement as an ongoing programme rather than a one-off request. Health systems are increasingly scrutinising the credibility of supply chain data, not just whether it exists.
4. Build a carbon reduction plan that will hold across multiple markets. Requirements are tightening on a fixed timeline and across more jurisdictions simultaneously. Build global emissions coverage from the start, with a clear reduction trajectory and methodology that holds up to procurement scrutiny across multiple customers, not just one health system.
Building the sustainability infrastructure healthcare requires
Building a credible carbon programme for healthcare procurement is not a one-time exercise. Requirements are tightening on a fixed timeline, and the organisations best placed to meet them are the ones that have already built the infrastructure: granular Scope 3 data, structured supplier engagement, and reporting that holds up to scrutiny.
Zevero helps healthcare suppliers build and maintain that infrastructure, from initial baseline through to product-level carbon footprinting and multi-jurisdiction reporting. Talk to our team to find out where to start.
See how Zevero can streamline your carbon reporting



